Nice ad! 
You are using an out of date browser. It may not display this or other websites correctly.
You should upgrade or use an alternative browser.
You should upgrade or use an alternative browser.
Best new intern stories: let em spill
- Thread starter opr8n
- Start date
- Joined
- Feb 4, 2014
- Messages
- 436
- Reaction score
- 290
I once (as a 2nd resident) was assisting my intern in placing a subclavian on a little old 70 yr DNR/I lady. Informed consent had been obtained. Somehow either the intern or I caused a pneumothorax and pt started desating to 60s. I called my attending who had the fellow place a pigtail catheter. It though didn't help pt still desating and needing constant bagging. Attending shrugged and said nothing could be done and stepped out for the day with pt still being bagged.
As soon as he left I spoke with family and convinced them to rescind DNR/I and intubated the pt with sats 40s. Called attending after intubation and told him family changed their mind. He shrugged again.
She lived although needed to go to nursing home for a while. She wasn't happy about being intubated but it was all kosher as family had rescinded the DNR.
As soon as he left I spoke with family and convinced them to rescind DNR/I and intubated the pt with sats 40s. Called attending after intubation and told him family changed their mind. He shrugged again.
She lived although needed to go to nursing home for a while. She wasn't happy about being intubated but it was all kosher as family had rescinded the DNR.
- Joined
- Apr 1, 2017
- Messages
- 255
- Reaction score
- 667
I once (as a 2nd resident) was assisting my intern in placing a subclavian on a little old 70 yr DNR/I lady. Informed consent had been obtained. Somehow either the intern or I caused a pneumothorax and pt started desating to 60s. I called my attending who had the fellow place a pigtail catheter. It though didn't help pt still desating and needing constant bagging. Attending shrugged and said nothing could be done and stepped out for the day with pt still being bagged.
As soon as he left I spoke with family and convinced them to rescind DNR/I and intubated the pt with sats 40s. Called attending after intubation and told him family changed their mind. He shrugged again.
She lived although needed to go to nursing home for a while. She wasn't happy about being intubated but it was all kosher as family had rescinded the DNR.
Seems like a blatant violation of medical ethics.
- Joined
- Feb 4, 2014
- Messages
- 436
- Reaction score
- 290
Yes. It was more than a decade back and I did not have the foresight to ask at that time. That and the experience of a Vtach/Vifib arrest during another line now makes me always get the DNR rescinded if possible for a procedure. At my current place anesthesia/surgery won't take a pt to OR without the DNR order rescinded for the duration of the procedure and for a reasonable period afterward to deal with any unexpected complications.
I have seen surgeons have respiratory complications post surgery on DNR/I pts wait till pt is unconscious ; get family to rescind DNR and then intubated the pt to deal with complications. I saw the pt a month later and she applauded the surgeon and her daughter for saving her life and vowed to be a full code from then on. It in the end all depends on how you communicate to family. Not everything is written in medical ethics books.
I have seen surgeons have respiratory complications post surgery on DNR/I pts wait till pt is unconscious ; get family to rescind DNR and then intubated the pt to deal with complications. I saw the pt a month later and she applauded the surgeon and her daughter for saving her life and vowed to be a full code from then on. It in the end all depends on how you communicate to family. Not everything is written in medical ethics books.
- Joined
- Jun 11, 2013
- Messages
- 11,528
- Reaction score
- 27,453
Yes. It was more than a decade back and I did not have the foresight to ask at that time. That and the experience of a Vtach/Vifib arrest during another line now makes me always get the DNR rescinded if possible for a procedure. At my current place anesthesia/surgery won't take a pt to OR without the DNR order rescinded for the duration of the procedure and for a reasonable period afterward to deal with any unexpected complications.
I have seen surgeons have respiratory complications post surgery on DNR/I pts wait till pt is unconscious ; get family to rescind DNR and then intubated the pt to deal with complications. I saw the pt a month later and she applauded the surgeon and her daughter for saving her life and vowed to be a full code from then on. It in the end all depends on how you communicate to family. Not everything is written in medical ethics books.
I'm not sure that is a great policy either.
- Joined
- Feb 4, 2014
- Messages
- 436
- Reaction score
- 290
Clinical judgement has to be exercised. A patient who is DNR/I and develops Vtach/fib during a central line placement clearly has a reversible condition that can be reversed with defibrillation/single round of CPR. Better if this possible complication and options were discussed prior to line placement but if it wasn't and V fib happens I will always give the benefit of the doubt, defibrillate and explain to patient/family later. I would think twice about placing IJ/SC if the patient told me specifically not to defibrillate in case of V Tach/Fib from ectopy during line placement.
That is in contrast to a patient with metastatic cancer on 4th line chemotherapy who is presenting with septic shock and is now on 4 pressors and the family still wants to be ' full code ' . When he develops asystole I am probably not going to do CPR for 2 hours.
That is in contrast to a patient with metastatic cancer on 4th line chemotherapy who is presenting with septic shock and is now on 4 pressors and the family still wants to be ' full code ' . When he develops asystole I am probably not going to do CPR for 2 hours.
- Joined
- Dec 23, 2013
- Messages
- 340
- Reaction score
- 340
I think it's horrifically unethical to mandate reversal of DNR/DNI during surgery or a procedure. The patient has expressed their wishes; it's unfortunate that you have a death on your record if they code during the case or the procedure, but why would they not want CPR in general but want it in the OR? Ridiculous thought process that I've never understood.
- Joined
- Sep 14, 2006
- Messages
- 23,863
- Reaction score
- 46,145
I think you would go that far in terms of it being a forced thing. However, if you have the conversation and discuss the possibility of very reversible causes and the patient chooses to allow things that is perfectly ethical. Just doing what you want or forcing people to do what you want should be universally considered unethical.I don't know that I would go that far.
An acute event perioperatively has a much different inciting cause, and usually a much better prognosis.
I think in many cases it is appropriate to reverse a DNR. But the conversation needs to be had in advance and handled ethically. Waiting for a patient to become unconscious and then violating their wishes is a huge ethics violation. The fact that one patient was okay that it happened doesn't mean it's appropriate.
- Joined
- Feb 4, 2014
- Messages
- 436
- Reaction score
- 290
I did not feel that good about the surgeon's decision to rescind the DNR/I after discussion with the daughter once the patient was not able to make her decisions. He probably did not want a perioperative mortality on his record. I actually signed off or rather the surgeon told me he wanted to manage the patient alone. I am pointing out that in real life often medical ethics doesn't work and a decision reached by family/physician will override medical ethics.
Families can be persuaded. 99% of the time if the physician requests that a DNR/I be reversed temporarily for a procedure the family will agree. And my feeling is that it is not wrong, it just gives the surgeon / anesthesia the ability to perform the procedure in the best possible manner without worrying about oversedation or ectopy.
Families can be persuaded. 99% of the time if the physician requests that a DNR/I be reversed temporarily for a procedure the family will agree. And my feeling is that it is not wrong, it just gives the surgeon / anesthesia the ability to perform the procedure in the best possible manner without worrying about oversedation or ectopy.
- Joined
- Sep 14, 2006
- Messages
- 23,863
- Reaction score
- 46,145
Ah, thought you meant the horribly unethical part.I meant specifically I wouldn't go that far as to call it a "ridiculous thought process"
- Joined
- Apr 27, 2004
- Messages
- 12,204
- Reaction score
- 7,337
Well I don't think many actually "force" a reversal of dnr but what about simply refusing to operate on someone who does not wish to pause or reverse the dnr? I think that's a more interesting ethical question. In some ways I can see how that is coercive but at the same time insisting I operate with my options limited doesn't seem right. I guess you could imagine a parallel to jehovahs witnesses. Should I be required to do a complex operation without the "safety net" of being able to use the full resources at my disposal to salvage a bad outcome?I think you would go that far in terms of it being a forced thing. However, if you have the conversation and discuss the possibility of very reversible causes and the patient chooses to allow things that is perfectly ethical. Just doing what you want or forcing people to do what you want should be universally considered unethical.
I do think there is some aspect of the "death on my record" disincentive which doesn't seem like good ethical reasoning but I'm sure plays into it somewhat.
- Joined
- Apr 27, 2004
- Messages
- 12,204
- Reaction score
- 7,337
Right. Medical ethics isn't like some sort of fool proof safeguard against wrongdoing, it is the standard by which we judge whether wrongdoing was done. And occasionally a toolkit for reasoning through problems.Saying that someone did something unethical isn't the same thing as "in real life often medical ethics doesn't work"
His example isn't a failure of "medical ethics" it's a failure of "the guy who taught that surgeon medical ethics"
- Joined
- Sep 14, 2006
- Messages
- 23,863
- Reaction score
- 46,145
I suppose I mean forced in the sense of in places where policy rescinds it without discussion or if the surgeon/anesthesiologist rescinds it without discussing it. Similarly I wouldn't want the surgeon or anesthesiologist forced to provide services if something they feel is a key component won't be allowed. But I think respectful discussion is highly likely to lead to compromise that all parties can feel ok with. This is as opposed to a unilateral declaration without delving into wishes and reasoning on both sides. And for situations where time is not of the essence referral to someone whose thoughts better align with the patient may be reasonable.Well I don't think many actually "force" a reversal of dnr but what about simply refusing to operate on someone who does not wish to pause or reverse the dnr? I think that's a more interesting ethical question. In some ways I can see how that is coercive but at the same time insisting I operate with my options limited doesn't seem right. I guess you could imagine a parallel to jehovahs witnesses. Should I be required to do a complex operation without the "safety net" of being able to use the full resources at my disposal to salvage a bad outcome?
I do think there is some aspect of the "death on my record" disincentive which doesn't seem like good ethical reasoning but I'm sure plays into it somewhat.
- Joined
- Feb 4, 2014
- Messages
- 436
- Reaction score
- 290
Medical ethics can be nebulous. What I have been taught is that in every situation you do what feels right to you and make a decision you can live with afterwards. I don't think any physician wakes up any day wanting to be the ' angel of death ' .
Another example : a young person comes with methanol overdose. Given fomepizole. It helps but super high methanol levels meeting criteria for hemodialysis. Alert /oriented and coherently declares that she is in sane mind and wants no hemodialysis. She gets nurses / charge nurse on her side and they are refusing to be any part of hemodialysis. Attending and me now trying to figure out what to do. We keep giving fomepizole and wait till evening until new nurses come on. At that point we call anesthesia, sedate and intubate the patient, place mahurkar and do 24 hrs of hemodialysis. Once methanol level 0 we take catheter out, extubate the patient and send to psych.
Another example : a young person comes with methanol overdose. Given fomepizole. It helps but super high methanol levels meeting criteria for hemodialysis. Alert /oriented and coherently declares that she is in sane mind and wants no hemodialysis. She gets nurses / charge nurse on her side and they are refusing to be any part of hemodialysis. Attending and me now trying to figure out what to do. We keep giving fomepizole and wait till evening until new nurses come on. At that point we call anesthesia, sedate and intubate the patient, place mahurkar and do 24 hrs of hemodialysis. Once methanol level 0 we take catheter out, extubate the patient and send to psych.
- Joined
- Sep 14, 2006
- Messages
- 23,863
- Reaction score
- 46,145
It isn't so much nebulous as you guys seeming to not care at all about patient autonomy and not really using medical ethics.Medical ethics can be nebulous. What I have been taught is that in every situation you do what feels right to you and make a decision you can live with afterwards. I don't think any physician wakes up any day wanting to be the ' angel of death ' .
Another example : a young person comes with methanol overdose. Given fomepizole. It helps but super high methanol levels meeting criteria for hemodialysis. Alert /oriented and coherently declares that she is in sane mind and wants no hemodialysis. She gets nurses / charge nurse on her side and they are refusing to be any part of hemodialysis. Attending and me now trying to figure out what to do. We keep giving fomepizole and wait till evening until new nurses come on. At that point we call anesthesia, sedate and intubate the patient, place mahurkar and do 24 hrs of hemodialysis. Once methanol level 0 we take catheter out, extubate the patient and send to psych.
Seems like you guys like the "commit battery first then hope no one minds" approach.
- Joined
- Sep 14, 2006
- Messages
- 23,863
- Reaction score
- 46,145
If she lacked capacity it would be easy enough to document this and do what is needed. The fact they waited until the nurses left makes me wonder if the patient truly lacked capacity.That's not nebulous at all - patient pretty clearly lacked capacity to refuse in that circumstance. It was particularly poorly handled though.
Your strategy of knock em out and do what we want after is a concerning pattern.
- Joined
- Feb 4, 2014
- Messages
- 436
- Reaction score
- 290
Well a patient who came in with a suicide attempt lacks capacity by definition no matter how eloquently she could state she was in her senses. As long as she had drunk the methanol at home and kept it to herself, she could do whatever she liked but once she came into our care stating she drank methanol, it was on us. The nurses were stupid enough to take her word that she was competent. We as the physicians weren't gonna be fooled. And if she was not going to cooperate with us for a hemodialysis catheter / hemodialysis we were within our rights to use physical and chemical restraints to make sure she got appropriate treatment and avoid danger to her and caregivers. Yes we were creative about waiting till evening shift but what can you do when staff won't cooperate.
How many times do we intubate and sedate trauma/inebriated patients to get imaging/ CTs ?
I am not sure of all the particular circumstances in this case but some of our ICU nurses were really dumb at that point. Somehow that patient was also able to play up a racial angle that put all the nurses on her side. On other occasions we were able to document two physician opinions for necessity of treatment.
How many times do we intubate and sedate trauma/inebriated patients to get imaging/ CTs ?
I am not sure of all the particular circumstances in this case but some of our ICU nurses were really dumb at that point. Somehow that patient was also able to play up a racial angle that put all the nurses on her side. On other occasions we were able to document two physician opinions for necessity of treatment.
Last edited:
- Joined
- Sep 14, 2006
- Messages
- 23,863
- Reaction score
- 46,145
In my state it doesn't require two doctors. One doctor can document incapacity which would then open the door for getting consent from family. If attempts to contact family fail then the doctor can document the life or limb threat and proceed with appropriate interventions. If nursing won't participate you get the charge. If that doesn't work you get the nursing admin. If that doesn't work you get ethics. If they go against you then you need to reevaluate if your position is correct. By skipping all that it makes it seem like you don't think your position is correct (which it might not be since it sounds like the issue was not life threatening at the time so even if you decide the patient lacks capacity you would still need to find next of kin to obtain consent). Instead if just waiting and doing it shady you could have done it appropriately if you are confident in your assessment of capacity and the need for the procedure.I mean there's about a million options there.
You document inability to consent and then document two physician consent for the necessity of treatment (that's the legal standard in my state, as it's been taught to me).
If the nurses don't agree?
Talk to Charge nurse, unit manager, risk management or office of patient safety or whatever it's called at your hospital. Get a psych consult if needed to document lack of consent. Ethics consult. Etc.
The option of waiting for the objecting nurses to leave is ethically unacceptable because you put the patient at risk by delaying therapy
- Joined
- Apr 27, 2004
- Messages
- 12,204
- Reaction score
- 7,337
Shouldn't it concern you a bit that the reaction you are getting seems to be uniformly shock and displeasure at the approach you seem to be taking? If these things were as nebulous as you suggest shouldn't your reaction be at least a little more mixed?
- Joined
- Feb 4, 2014
- Messages
- 436
- Reaction score
- 290
Why everyone's reaction to 3 cases is shock/displeasure where the doctors felt that their duty was to preserve human life I am not sure about. One case is of a potentially reversible complication of a central line placement requiring intubation , the other is a no - brainer indication for hemodialysis with a methanol level > 200. Both cases were complicated since in 1 the management of an adverse complication was not discussed prior and in the other case a rather persuasive patient managed to get nursing staff on her side. In neither case the patient was left with a lasting disability.
I think the surgeon should have honored his patients wishes but a month down the line she was happy with her surgeon and her family for the decision they made so it's difficult for me to question what he did.
DNR/I are fluid. So many times I have seen pt telling me they are DNR/I and then reverse themselves and say they wanted at least intubation if my expectation was that it would be a short term thing but they would not want themselves resuscitated if there is ' no hope '.
I dislike DNR/Is when I recognize I am doing a procedure that has known complications but potentially reversible with CPR/intubation. Just as I would not want to do a liver transplant in a patient who does not want me to give him blood transfusions.
I think the surgeon should have honored his patients wishes but a month down the line she was happy with her surgeon and her family for the decision they made so it's difficult for me to question what he did.
DNR/I are fluid. So many times I have seen pt telling me they are DNR/I and then reverse themselves and say they wanted at least intubation if my expectation was that it would be a short term thing but they would not want themselves resuscitated if there is ' no hope '.
I dislike DNR/Is when I recognize I am doing a procedure that has known complications but potentially reversible with CPR/intubation. Just as I would not want to do a liver transplant in a patient who does not want me to give him blood transfusions.
Last edited:
- Joined
- Apr 27, 2004
- Messages
- 12,204
- Reaction score
- 7,337
Yes well I dislike Catholicism and also red licorice. Your dislike for dnr has literally nothing to do with it.
- Joined
- Feb 27, 2005
- Messages
- 3,617
- Reaction score
- 5,206
I miss when this thread was about intern silliness/gaffs.
- Joined
- Feb 4, 2014
- Messages
- 436
- Reaction score
- 290
Well I dislike DNR/Is when someone gets transferred to ICU and needs aggressive interventions in 1st 2 days. It's like asking me to put a line with one hand tied behind my back. If you want me to give it my best shot at making you better let me give it my best shot. Let's go aggressive and after a couple of days we can reevaluate.
- Joined
- Jun 15, 2004
- Messages
- 1,305
- Reaction score
- 1,366
I miss when this thread was about intern silliness/gaffs.
Related to interns and coding...
I was nearby in an ICU when an intern hopped up and started doing compressions on a patient. The patient bolts upright and goes "What the hell!?" As it turns out, the harness for the monitor was loose causing the patient to "flatline".
- Joined
- Jun 8, 2008
- Messages
- 2,495
- Reaction score
- 3,860
Exam skills are very poorly taught in medical school these days.
It was poorly taught in the old days too. The only difference is we have technology these days to make up for our poor exams, so people don't die as often.
- Joined
- Apr 27, 2004
- Messages
- 12,204
- Reaction score
- 7,337
Most memorable senior wisdom I got as an intern:
I was in house call and the chief happened to be in house as well, I got called to the ed to see a patient, this had to have been first or second call, so early July. I think they had like acute cholecystitis or some other similar issue (i.e. not emergently operative or dying) but they are having a lot of pain. So I do my h&p thing, and give the patient probably like 0.5 of morphine so as not to kill them, patient continues to complain of pain. So I call my senior saying listen this lady has ACUTE CHOLECYSTITIS with a wbc of 16! I gave her morphine and abx and she isn't better!! What should I do?
He looks at me, says "sounds like she needs a doctor" and walks away.
Same chief, month or two later, trauma service, drunk with large facial lac he tells me to go repair it. I spend like 2 hrs sewing this guys face up, he was drunk and not exactly a cooperative drunk, I'm dripping sweat and exhausted and as I'm throwing last stitch my senior walks by and says "looks pretty good but we don't use vicryl on the face." So I started over.
I was in house call and the chief happened to be in house as well, I got called to the ed to see a patient, this had to have been first or second call, so early July. I think they had like acute cholecystitis or some other similar issue (i.e. not emergently operative or dying) but they are having a lot of pain. So I do my h&p thing, and give the patient probably like 0.5 of morphine so as not to kill them, patient continues to complain of pain. So I call my senior saying listen this lady has ACUTE CHOLECYSTITIS with a wbc of 16! I gave her morphine and abx and she isn't better!! What should I do?
He looks at me, says "sounds like she needs a doctor" and walks away.
Same chief, month or two later, trauma service, drunk with large facial lac he tells me to go repair it. I spend like 2 hrs sewing this guys face up, he was drunk and not exactly a cooperative drunk, I'm dripping sweat and exhausted and as I'm throwing last stitch my senior walks by and says "looks pretty good but we don't use vicryl on the face." So I started over.
- Joined
- Feb 27, 2005
- Messages
- 3,617
- Reaction score
- 5,206
Lol at @vhawk. Seniors/chiefs. Sometimes so helpful, sometimes not. I recall as an intern being tasked with replacing an old balloon gastrostomy in the ED. Patient had had one forever, it came out so they came to ED. I'm tasked with going to materials to get a new balloon gastrostomy. The materials people aren't particularly helpful so I end up coming back with a balloon GJ because they couldn't/wouldn't help me find the plain Gtubes and honestly I'm green enough I don't quite know the difference. Senior says that's alright we'll just cut off the J part. So he snips that off and we install it and blow up the balloon but it doesn't stay put. So we pull it back out and I'm looking at the end and say "I think you cut the balloon" as he is pushing saline through the balloon port to test it and sprays me in the face with a mixture of saline and the gastric juices that were on the thing. At that point I just look at him balefully and say "I have another consult to see. Do you want to see if you can get the right tube from materials?" Given I had gastric juice and saline running down my face he agreed that might be a good division of labor.
This is my absolute favorite intern story. A gen surg prelim intern was on the ortho service. He was told to do a wet-to-dry kerlix dressing on one of the hand infection patients. He said no problem, and was gone for 30 minutes. When he came back he confided to an ortho intern he didn't know how to do the dressing and couldn't figure it out, so the ortho intern proceeded to spend 10 minutes explaining how to do a wet-to-dry dressing. 45 minutes later he comes back and says he's not sure if he did it right to the ortho intern. Senior is now suspicious this has taken a good hour and a half to accomplish goes to investigate.
When the senior walks in the room, the entire floor is covered in small puddles of water. The patient, the gown and the patient's bed are soaked wet. The patient looks slightly terrified and has a giant mound of wet kerlix on top of his hand.
When the senior walks in the room, the entire floor is covered in small puddles of water. The patient, the gown and the patient's bed are soaked wet. The patient looks slightly terrified and has a giant mound of wet kerlix on top of his hand.
- Joined
- Apr 27, 2004
- Messages
- 12,204
- Reaction score
- 7,337
Ha thats pretty good. We had to transition to calling them "damp to dry" dressing changes for similar incidents to thisThis is my absolute favorite intern story. A gen surg prelim intern was on the ortho service. He was told to do a wet-to-dry kerlix dressing on one of the hand infection patients. He said no problem, and was gone for 30 minutes. When he came back he confided to an ortho intern he didn't know how to do the dressing and couldn't figure it out, so the ortho intern proceeded to spend 10 minutes explaining how to do a wet-to-dry dressing. 45 minutes later he comes back and says he's not sure if he did it right to the ortho intern. Senior is now suspicious this has taken a good hour and a half to accomplish goes to investigate.
When the senior walks in the room, the entire floor is covered in small puddles of water. The patient, the gown and the patient's bed are soaked wet. The patient looks slightly terrified and has a giant mound of wet kerlix on top of his hand.
This is my absolute favorite intern story. A gen surg prelim intern was on the ortho service. He was told to do a wet-to-dry kerlix dressing on one of the hand infection patients. He said no problem, and was gone for 30 minutes. When he came back he confided to an ortho intern he didn't know how to do the dressing and couldn't figure it out, so the ortho intern proceeded to spend 10 minutes explaining how to do a wet-to-dry dressing. 45 minutes later he comes back and says he's not sure if he did it right to the ortho intern. Senior is now suspicious this has taken a good hour and a half to accomplish goes to investigate.
When the senior walks in the room, the entire floor is covered in small puddles of water. The patient, the gown and the patient's bed are soaked wet. The patient looks slightly terrified and has a giant mound of wet kerlix on top of his hand.
Haha, that's great.
This reminds me of a story about a prelim surgery intern in my intern class back in the day. He was on the trauma surgery service at the time, and was told to go remove staples from a patient's belly incision. For some reason, he decided that this meant he should remove every staple in the patient's skin, including those in Ortho's post-op day 1 fasciotomy closures in the patient's legs.
The Ortho attending then walks in the room a couple hours later to find giant dehisced wounds where his nice fasciotomy closures used to be. The Ortho attending, who was notably unpleasant to deal with, searches out the prelim intern to chew him out for 10 minutes. Once he is finished and storms off, the intern runs down the hall after him to apologize, after which the attending starts up again and continues to scream at the intern for another 10 minutes in the middle of the nurses station.
- Joined
- Jun 4, 2007
- Messages
- 11,612
- Reaction score
- 836
I'm now a vascular fellow but obviously we have various interns rotating on our service. This weekend I was rounding with my attending when this intern who is crosscovering rushes up to us out of breath and sweating to tell us a particular patient has a PE and OMG maybe they have cholecystitis. He goes on and on about the gallbladder and the consult for it. He basically paints it like this patient is dying from both PE and cholecystitis.
He walks away and my attending is like "who is that?" Then, we go see the patient after his frantic outburst. Lady is the cutest grandmother peacefully sleeping in bed. We wake her up and she is smiling and totally asymptomatic. I see the general surgery note later in the day signing off bc she has no abdominal pain.
He walks away and my attending is like "who is that?" Then, we go see the patient after his frantic outburst. Lady is the cutest grandmother peacefully sleeping in bed. We wake her up and she is smiling and totally asymptomatic. I see the general surgery note later in the day signing off bc she has no abdominal pain.
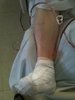
During my general surgery years, I was rotating at the VA. One of our postoperative patients with a 1st toe amputation for wet gangrene had been transferred back to the medicine service because he had a thousand medical problems. At 8 am we get a call from the medicine service. They said that his wound VAC isn't working. The overnight medical chief resident rewrapped the wound VAC and it isn't working. We go to see the patient and see this. I had to walk out of the room so I didn't laugh in front of the patient but had to come back in to snap a pic.
Attachments
- Joined
- Jun 15, 2004
- Messages
- 1,305
- Reaction score
- 1,366
They said that his wound VAC isn't working. The overnight medical chief resident rewrapped the wound VAC and it isn't working. We go to see the patient and see this. I had to walk out of the room so I didn't laugh in front of the patient but had to come back in to snap a pic.
While I no doubt find this amusing, I would suggest you remove the picture from your post and keep a text description. While there isn't any identifiable information, I do know that the VA has some fairly strict policies regarding photography.
Similar threads
- Replies
- 2
- Views
- 768